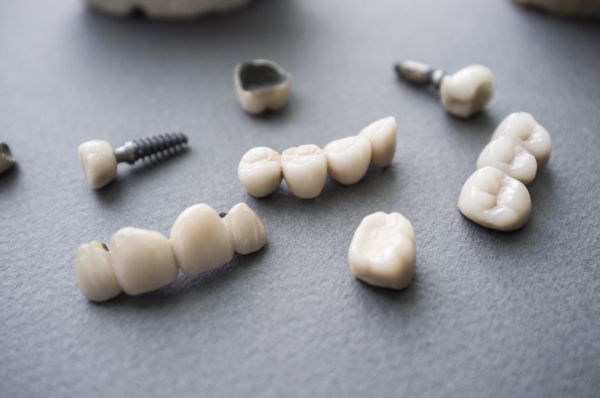
It is estimated that in 2018, the dental implant market is projected to reach over $6.4M in the United States. It appears that everyone is jumping onto the implant bandwagon; however, dental implants may not always be the best solution. One of my former teachers said, “I can put an implant anywhere… ANYWHERE!” However, careful planning is always required when considering an implant. There are several factors that can add to or detract from implant success. Regardless of what you may have heard, based on existing research, implants do not have 100% success, and in some cases it may be more prudent to save a tooth.
Medical/Social factors
There are multiple factors that contribute to the success of implants, but foremost are medical and social history. There are certain medical conditions that would either preclude you from dental implants or place you at risk of implant success. Of these, blood, bone, collagen, and other metabolic disorders are contraindications for implants. Social histories that include smoking tend to increase implant failure rate. Consult with your surgeon for further clarification.
Intra-oral factors
There are specific intra-oral factors that can influence implant success, one of which is location in the mouth. Functional demands placed on implants vary in the front or the back of the mouth as well as upper versus lower jaw. The bone density in the posterior sections of the upper jaw tends to be less and because it is closer to the chewing muscles, they receive the greatest amount of force. Contrast that to the front of the mouth, where bone tends to be comparatively denser; yet the functional demands are less. Although the front of the mouth may be functionally more favorable, the additional challenge with upper anterior implants is esthetics. Specific gum biotypes are more prone to recession and can lead to esthetic implant failures. However, all the above are moot if there is insufficient bone height, width, or density. Additionally, if excessive functional demands are placed on implants, there is a risk of failure of the crown on the implant or of the implant body.
Secondary factors
Secondary factors that can influence long-term implant success include having an adequate zone of gum tissue hugging the collar of the implant, which is true for natural teeth as well. An inadequate zone would lead to accelerated bone loss around the implant. Some research studies also indicate that the thickness of gum tissue surrounding the implant helps prevent bone loss. Other studies indicate that the bacteria makeup associated with teeth are still present even after teeth are extracted and therefore can influence the microbiology around the implants. There has also been research suggesting that there is release of titanium ions into the gum tissues surrounding the implant, leading to a low-grade inflammatory process in the gums, which may be exacerbated in the presence of biting trauma leading to accelerated bone loss.
In Conclusion, Is it worth it?
Undoubtedly, dental implants have revolutionized the way dentists can treat patients, and in certain situations, implants would be the ideal choice of treatment, but we also need to ask if saving a natural tooth may be better in the long term. In my opinion, implants should be used as an adjunct to treatment. A discussion with your dentist or implant surgeon is paramount, for there may be more to your implant than simply placing a screw into the bone.
Dr. Scott Nakamura maintains a practice at: Exton Medical Arts Building 80 W Welsh Pool Rd, #207 Exton, PA 19341 (610) 636-5997 |